 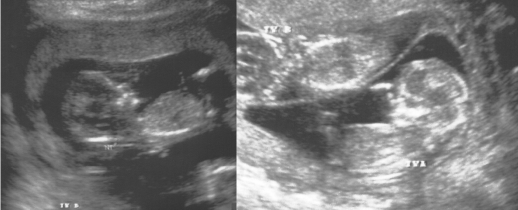
Our data suggest that the combination of nuchal translucency measurement in the first trimester and the triple test in the second trimester is associated with a very high detection rate of trisomy 21 at a relatively low screen-positive rate. In comparison, screening by maternal age alone would have identified nine (47%) trisomy 21 pregnancies with a screen-positive rate of 10.7%. Soft markers were originally introduced to prenatal ultrasonography to improve the detection of trisomy 21 over that achievable with age-based and serum screening strategies. From 2009 to 2016, we studied 72 pregnant women with fetal nuchal fold (NF) measurements over 5 mm at 14 to 19 + 6 weeks or 6 mm at 20 to 28 weeks of gestation who received prenatal diagnosis. Two sequential screening approaches, stepwise and contingency, have been introduced to allow disclosure of results in the first trimester. increased NT seen at a first trimester ultrasound for Down syndrome screening. The key factor that has allowed testing during the first trimester is the ultrasonic measurement of the Nuchal fold translucency (NT) thickness. To summarize the results of prenatal diagnoses and pregnancy outcomes of fetuses with thickened nuchal fold (TNF) in the second trimester. to as nuchal skin fold) in the first trimester of pregnancy has become an. The detection rate using the combined screening method was 95% (18/19) with a screen-positive rate of 7.2%. This test is available from week 11, day 0 through week 13, day 6 of gestation. When this marker is combined with concurrent maternal serum markers, the model-predicted performance is greater than for all second-trimester serum-only combinations. Amniocentesis was offered to women in whom the nuchal translucency was 2.5-3.4 mm, the triple test showed a risk of > or = 1 : 250 and in women aged > or = 35 years. Nuchal translucency is the single most discriminatory marker for screening Down syndrome. In practice, however, many women also receive sequential ultrasound screening, having a second-trimester anomaly scan 5. 
All other women were asked to return for the triple test at 16 weeks' gestation. The most widely promoted sequential screening strategies of this type are based on second-trimester serum markers, tested on most (‘step-wise’) or only a small proportion (‘contingent’) of those screened in the first trimester 4. A nuchal translucency scan was carried out at 10-13 weeks' gestation and for those with a measurement of 3.5 mm or more chorionic villus sampling was performed. This was a retrospective study of 9342 women with singleton pregnancies who booked for delivery in our hospital over a period of 5 years. An association between an abnormally thickened nuchal translucency (NT) and chromosomal abnormalities was first noted in the early 1990s1. To evaluate screening for trisomy 21 in a low-risk population utilizing a combination of nuchal translucency measurement in the first trimester and the triple test in the second trimester. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
